

Written by: Maria-Elizabeth Baeva, Jefferies Lab alum (right)
Edited by: Andy An, MD/PhD Student, Hancock Lab (left)

Here’s a paradox: I am a medical student who dreads going to a new hospital. Why? Because inevitably I will get lost. Many other people are also anxious about going to a hospital. Beyond the association with illness, healthcare settings tend to be cold, unwelcoming, and confusing areas. But why?
This sister article to my previous piece on laboratory space design hopes to shed light on this often-overlooked aspect of healthcare: design. If you are skeptical about the effects of design on our wellbeing, then think about this: hospitals with more operating rooms have been shown to perform more Caesarean sections1. The way our buildings are structured quite literally could impact us from the day we are born.
-
This blog is the second in a two-part series about the design of scientific spaces. Read the first blog, focused on the design of laboratory spaces: “No Home for My Genome (Sequencing Apparatus): Special Considerations for Laboratory Design”
Architecture
Hospital architecture has changed dramatically over the course of 150 years. While it may be tempting to assume that these buildings are designed with an objective and utilitarian goal in mind, the culture and values of the people surrounding the hospital often have more sway on its design. Victorian hospitals were designed with ventilation in mind and were styled as half-and-half institution and residence, whereas its antecedent, the interwar modern hospital, was focused much more on efficiency and thus crammed more utilities, rooms, and equipment into its allocated space2. The postwar modern hospital is the “classical” hospital design we think of with its white and sterile hallways2. But now, new postmodern hospitals have introduced more color and resemble airports or shopping malls in terms of aesthetics2. It will be interesting to see how hospitals continue to evolve in the next 150 years.
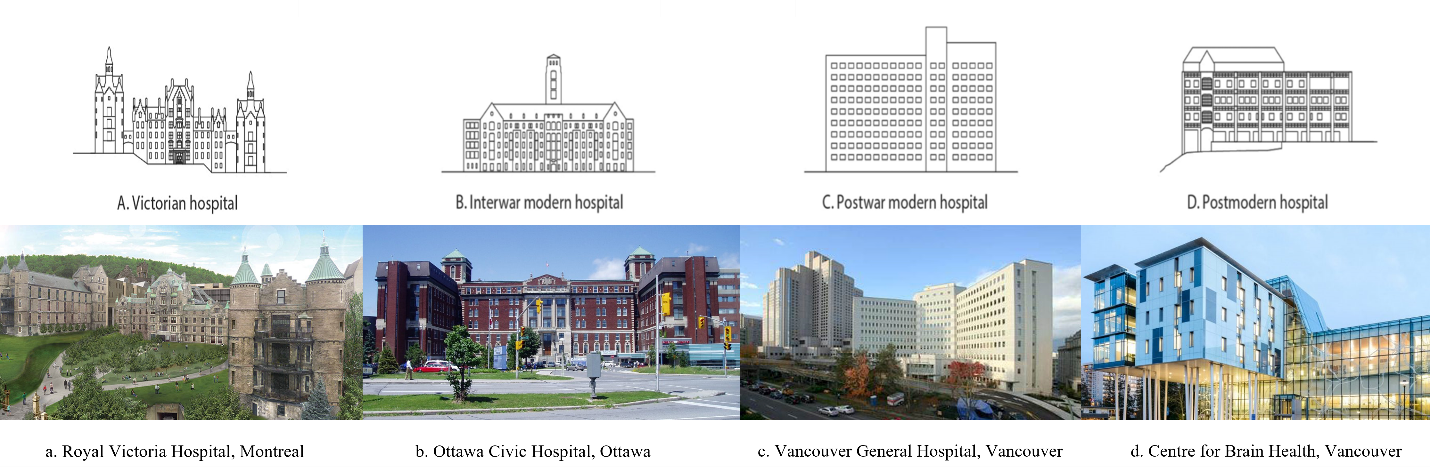
Figure 1. Canadian hospitals over the last 150 years. Adapted and modified from reference 2.
Lighting
We’ve all been awoken from a deep slumber by an annoying roommate or sibling turning on a light. Now imagine you are in the intensive care unit (ICU) where there is a constant and bright light while you are desperately trying to stay alive. A phenomenon known as “ICU psychosis” has been observed in both adults and children and has been partially attributed to this constant and unnatural disruption to our circadian rhythm, especially during a time when sleep is most critical3-5.
But bright lights are not all bad. As obvious as it may seem, having brighter lights in hospitals can prevent medical errors associated with visual tasks, such as dispensing medications6. Perhaps being mindful of where bright lights are necessary and where they can be dimmed can go a long way towards creating a more comfortable environment for both patients and healthcare providers.
Noise
Although shows like House or General Hospital show plenty of solemn and quiet moments with patients and physicians, the reality is that hospitals are very loud places. So loud in fact, that most hospitals have higher noise levels (50-100 dB) than what is recommended by the World Health Organization (<35 dB)7. For context, 100 dB is the sound of a car horn or power tool. High noise levels may also contribute to the previously noted ICU psychosis3,4.
And it’s not just patients feeling overstimulated: staff also report noise-induced stress. So, what can be done? Simple solutions such as using sound-absorbing instead of sound-reflecting ceiling tiles can decrease noise levels and have been shown to improve the working conditions (and thus the healthcare provided) of hospitals8.
Walking and wayfinding
Getting lost in a hospital may be one of the few truly universal human experiences. Hospitals are often very large and house many different departments, so an intuitive wayfinding process is a necessity. It is important to not only be mindful of how landscape, interior architecture/design, signage, graphics, and amenities can influence how easy it is to find a specific location, but also to incorporate many strategies so that everyone can find their way9,10. For example, including maps and written instructions for cognitively-focused individuals, volunteers to guide/talk to people for verbal communicators, and landmarks and colors for visual learners will make sure that fewer people are late to their appointments9,10.
But getting lost and walking long distances are not problems only for patients. Nurses, who spend almost a third of their day walking, feel fatigue and stress because they must walk long distances from one task to the next3.
Hospitals are often very large and house many different departments, so an intuitive wayfinding process is a necessity. It is important to not only be mindful of how landscape, interior architecture/design, signage, graphics, and amenities can influence how easy it is to find a specific location, but also to incorporate many strategies so that everyone can find their way.
Are there any real-world examples of intuitive wayfinding? This is where the principle of “progressive disclosure”9 becomes useful. This basically means that information is disclosed when needed instead of being given all at once. For example, your Google/Apple maps app doesn’t give you all the directions at once: rather it is given to you once you’ve reached a certain destination. Patients arriving at the hospital for the first time may find themselves overwhelmed with instructions, landmarks, and confusing corridors9. Instead, having a stepwise approach to wayfinding will make navigation much smoother and less stressful.
Bedspace
Finally, we arrive at the smallest but perhaps most intimate aspect of hospital design: the bedspace. There is overwhelming evidence that single rooms provide more benefit than multi-bedrooms: there is increased privacy, decreased noise11, less chance of spreading infection12, and more comfortable visits from families and loved ones. While sometimes a shared spaced is preferable (long-term elderly and pediatric patients can benefit from the company of others close by), having a private space for patients and their families is not only in keeping with a patient-centered approach to healthcare, but may also derive medical benefit as well: when families are involved in a patient’s healthcare, including discussion of medications and care plans, patient mortality decreases13. Isn’t that the ultimate goal of a place of healing – to simultaneously help the patient physically, mentally and emotionally?
Start from scratch?
With all this being said, does this mean we need to tear down all the hospitals built before 2022 and start again? Not at all. Instead, this means that we should take lessons and ideas that worked from the past, incorporate realistic and practical changes in the present, and be proactive and mindful in future hospital designs. As an example, St. Paul’s Hospital is undergoing redevelopment: check out their design page and see for yourself – they are incorporating the elements discussed here. And most importantly, we must not forget that the role of a hospital is a place of healing! So, it must be designed with the health, comfort, and wellbeing of both patients and staff in mind.
References
- (2017). Designing Capacity for High Value Healthcare: The Impact of Design on Clinical Care in Childbirth. MASS Design Group. Retrieved from https://massdesigngroup.org/sites/default/files/file/2017/170223_Ariadne%20Report_Final.pdf
- Adams, A. (2016). Canadian hospital architecture: how we got here. CMAJ 188 (5): 370-371. Doi: https://www.cmaj.ca/content/188/5/370
- Monks, RC. (1984). Intensive Care Unit Psychosis. Can Fam Physician 30: 383–388. Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2154033/
- Joseph A and Rashid M. (2007). The architecture of safety: hospital design. Curr Opin Crit Care 13: 714–719.
- Hughes J. (1994). Hallucinations following cardiac surgery in a pediatric intensive care unit. Intens Crit Care 10:209–211.
- Buchanan TL et al. (1991). Illumination and errors in dispensing. Am J Hosp Pharmacy 48: 2137–2145.
- Xyrichis A et al. (2018). Noise pollution in hospital.s BMJ 363: k4808. doi: 10.1136/bmj.k4808
- Blomkvist V et al. (2005). Acoustics and psychosocial environment in coronary intensive care. Occupat Environ Med 62: 1–8.
- Huelat BJ. (2007). Wayfinding: Design for Understanding. The Center for Health Design.
- Harper et al. Designing Wayfinding Systems for Hospitals (Poster). University of Houston Clear Lake. Retrieved from http://cms.hfes.org/Cms/media/CmsImages/Designing-Wayfinding-Systems-for-Hospitals.pdf
- Ulrich RS. (2006). Evidence-based health-care architecture. Lancet 368: S38–S39.
- Stall N. (2012). Private rooms: evidence-based design in hospitals. CMAJ 184: 162-3.
- Kuipers SJ et al. (2019). The importance of patient-centered care and co-creation of care for satisfaction with care and physical and social well-being of patients with multi-morbidity in the primary care setting. BMC Health Serv Res 19. Retrieved from https://doi.org/10.1186/s12913-018-3818-y


